Let’s face it. Open enrollment is the season of frustration and worry. Employees struggle to determine which plan is best for them, and HR professionals shoulder the burden of making sure they find it. And each season seems to bring a new curve ball, prompting yet another call to your broker or benefits consultant.
It’s time to do benefits differently.
Even the most amazing brokers and benefits consultants have a common limitation. It’s just not possible to take a deep dive into each employee’s distinct scenario. But it’s not for lack of trying.
The old model doesn’t scale.
The challenges facing modern organizations when it comes to scaling benefits are many, and the resources required have always been a lot. Year after year, employers struggle to do the following:
- Manage the renewal process
- Decide on the best plans
- Analyze available data, and
- Communicate changes—to an employee population that spans older adults, Millennials, people with chronic conditions, and healthy people (with or without dependents!)
“Change management” is a huge headache for HR.
The easy way out? Punt any plan design renewal to next year. Change management consumes time and resources, and brokers are unlikely to challenge this inertia. Brokers have no incentive to push an overhaul if you’re not up for it. So, for another year, the underlying issues remain.
Healthcare costs aren’t going down.
Rising healthcare costs continue to apply pressure on employers and employees alike. Both parties need to come together and consider alternatives. There needs to be a win/win.
Today’s brokers must heed a new calling.
Brokers must heed a new calling: proactively take on the fiduciary responsibility of mitigating rising costs. This is especially essential for small and mid-sized clients.
Technology and actionable insights are key.
To successfully scale benefits expertise, HRtech and data are foundational. Especially as you seek to engage employees who may be geographically distributed, working flexible hours, and looking for on-demand access to decisioning tools (the one-time open enrollment meeting with a dry powerpoint presentation just isn’t cutting it).
Employees have two burning questions.
Based on polling thousands of employees, the most common questions during open enrollment are:
- Are my doctors/providers in-network?
- What is the best-value plan for my needs?
In the past, answering these two questions would have been nearly impossible for an entire organization. Insight into a range of factors would have been required including, but not limited to:
- Existing prescriptions and healthcare issues
- Current healthcare providers
- Expected healthcare needs
- Dependent healthcare needs and healthcare providers
Lumity delivers 1:1 decisioning guidance.
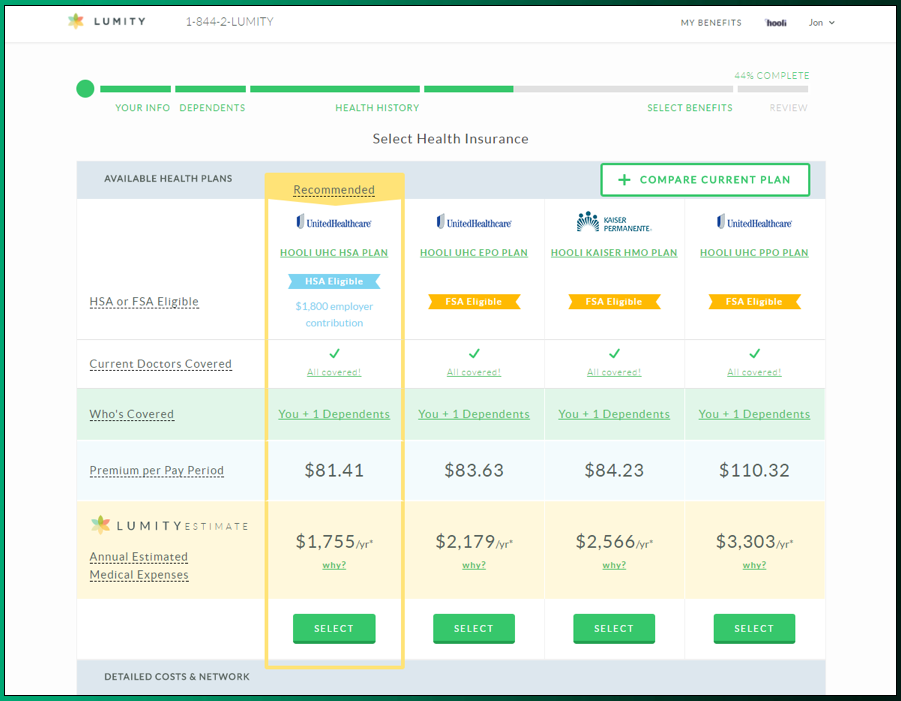
Lumity’s health benefits platform integrates with carrier provider databases. So, when choosing a plan, your employees know whether their doctors are in-network.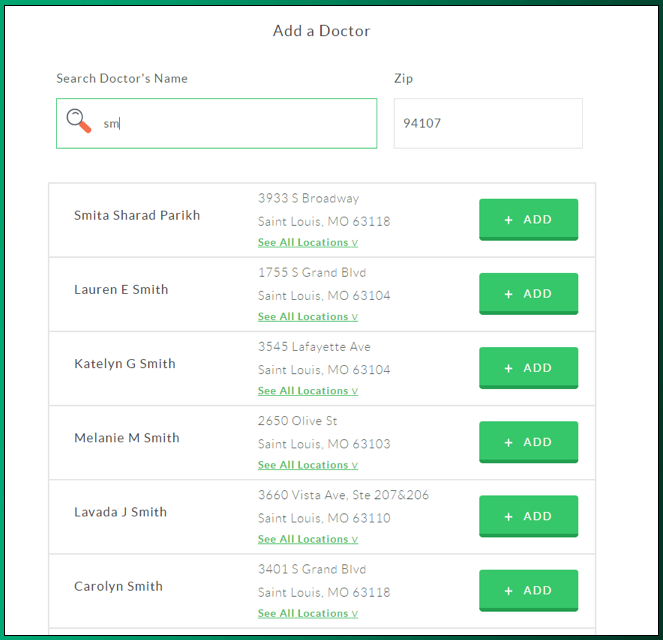 Lumity’s system plugs into all the national carriers. This means your company is no longer locked within the same carrier and renewal process. There are no more “change management” hassles.
Lumity’s system plugs into all the national carriers. This means your company is no longer locked within the same carrier and renewal process. There are no more “change management” hassles.  During open enrollment, not only can employees see how many of their doctors are in-network with each available medical plan offered, but they can see a value-based recommendation based on available information (age, gender, location, or Lumity risk profile). Employer contributions also play a crucial role providing the right incentives for a benefits strategy. Getting the contributions right is also why we play the 1:1 role of the trusted benefits advisor. The entire experience matters, from employer to the employee.
During open enrollment, not only can employees see how many of their doctors are in-network with each available medical plan offered, but they can see a value-based recommendation based on available information (age, gender, location, or Lumity risk profile). Employer contributions also play a crucial role providing the right incentives for a benefits strategy. Getting the contributions right is also why we play the 1:1 role of the trusted benefits advisor. The entire experience matters, from employer to the employee.
Prepare for a win/win.
It’s time for an easy change. Lumity built its business on optimizing health plan designs and advocating for you—and your employees. With Lumity, it's possible to contain costs while delivering improved benefits and a better enrollment experience to your employees. Contact us today. Related reading: Ending Renewal Roulette